Your Colorectal Health, Our Priority
With our comprehensive suite of screening services and treatment options, our experienced colorectal specialist and medical team promise you peace of mind whilst ensuring a strong and healthy colon.

Dr Ho Kok Sun
Consultant Colorectal & General Surgeon
MBBS (Singapore), M Med (General Surgery) (Singapore)
FRCS (General Surgery) (Edinburgh), FAM (Singapore)
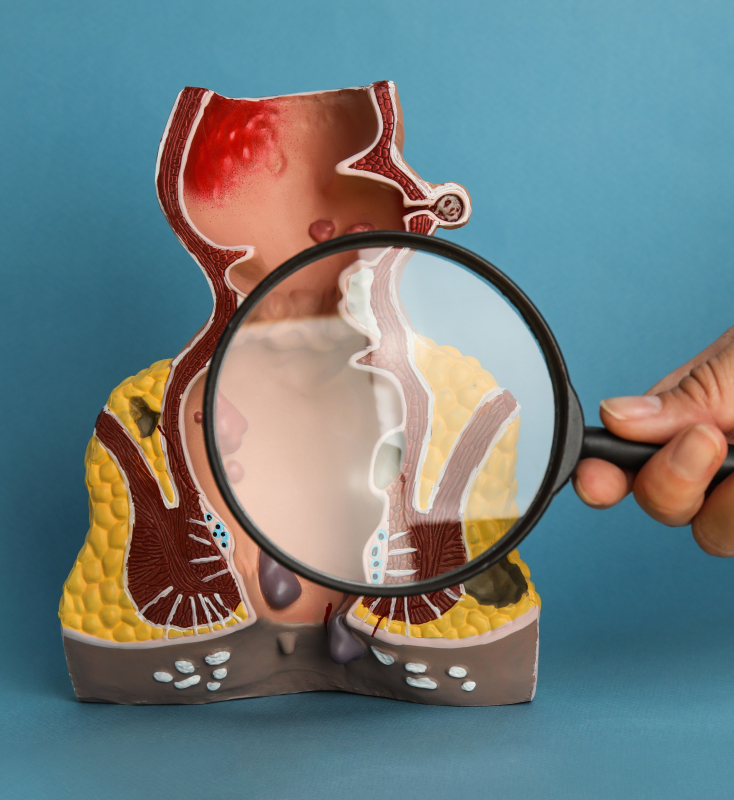
What ArePiles?
Haemorrhoids (or piles) are swollen blood vessels located in the anus. They can be classified as internal or external piles, depending on the location where they start.
Piles are commonly understood to form when repetitive straining causes a high pressure within the blood vessels. The wall of the blood vessel gets stretched and thinned out by this swelling, becoming more prone to breakage. Once this happens, bleeding occurs.
Repetitive straining also causes the supporting ligaments in the blood vessel to become overstretched and lose their elasticity. When the blood vessel loses elastic support, it descends further down the anal canal and protrudes outside of the anus.
Piles can cause a lot of discomfort and should be treated promptly through a method that works best for your specific type and severity of piles.
What Are the Different Types of Piles (Haemorrhoids)?
What Causes Piles To Form?
What Are Some Common Symptoms of Piles?
How Can I Tell If My Piles Are Serious?
What Happens if Piles Are Left Untreated?
More serious and symptomatic cases of piles should receive prompt medical attention to alleviate symptoms and prevent painful complications.
How Are Piles Diagnosed?
A doctor can diagnose piles or haemorrhoids by conducting a physical examination, where they will carefully inspect the anal region for any signs of piles: lumps or swelling, prolapsed haemorrhoids, external haemorrhoids, skin irritation, skin tags.
If the physical examination is not conclusive, additional tests may be performed to confirm the diagnosis. These include:
- Digital Rectal Exam - During the examination, the doctor will gently insert a gloved, lubricated finger into the patient’s rectum to check for the presence of internal haemorrhoids.
- Anoscopy - In this procedure, a thin, lighted tube (anoscope) is inserted into the anus to allow the doctor to visually inspect the lining of the lower rectum and anus and identify haemorrhoids or other abnormalities.
- Sigmoidoscopy - This test is similar to anoscopy, except that the doctor uses a specialised instrument called a sigmoidoscope to view the lower portion of the colon (sigmoid) and rectum and look for the presence of haemorrhoids.
How Do I Prepare for Piles Surgery?
- Follow Pre-Surgery Instructions - Before you begin the surgery process, your doctor will review your medical history, current medications and any existing conditions such as hypertension or diabetes, to ensure you are fit for surgery. Your doctor will advise when to stop eating or drinking before the operation, usually several hours beforehand. Certain medications, including blood thinners or supplements that affect bleeding, may need to be paused.
- Arrange Support and Transportation - Since piles surgery is often done under anaesthesia, patients are usually advised to arrange for someone to accompany them home after the procedure. Having assistance at home for a day or two can also be helpful during the initial recovery phase.
- Plan for Recovery at Home - Prepare your home for comfort and convenience after surgery. This may include having easy-to-digest foods, stool softeners (if prescribed) and items such as cushions for sitting. Keeping the bathroom clean and accessible can also support hygiene and comfort.
- Maintain Good Bowel Habits Before Surgery - A balanced diet rich in fibre and adequate hydration may help reduce constipation before surgery. Avoid straining during bowel movements, as this can worsen haemorrhoids or cause discomfort before the procedure.
- Ask Questions Before the Operation - It is advisable to discuss what to expect during and after surgery, including pain management, wound care and your recovery timeline. Understanding the procedure can reduce anxiety and help you prepare mentally and physically.
What Should I Expect During Piles Surgery?
Piles surgery, also known as haemorrhoidectomy, is usually performed under regional or general anaesthesia, so you will not feel pain during the procedure. The operation may be done as a day surgery, meaning most patients do not need to stay overnight.
During the procedure, the surgeon removes or treats the swollen haemorrhoidal tissue using techniques such as excision, stapling or ligation, depending on the type and severity of haemorrhoids. The goal is to relieve symptoms like bleeding, pain or prolapse.
After surgery, you’ll be moved to a recovery area for observation until the effects of anaesthesia wear off. Some discomfort, mild bleeding or swelling is common in the first few days. Your doctor will provide instructions for pain management, wound care and bowel habits to support healing.
What Are the Piles Treatments Available at Our Clinic?
Piles that do not cause any symptoms do not require piles surgery.
For first- or second-degree piles, symptoms can be relieved by reducing straining during bowel movement. This could mean taking more fluids or laxatives. Oral medication or suppositories may be given by your piles surgeon to relieve the symptoms.
If this does not help, further treatment may be required. This includes the following procedures:
- LigationThe rubber band treatment
- SclerotherapyAn injection is given to the area around the piles. This method is relatively painless and causes the piles to shrink.
- Ultrasound Guided Haemorrhoidal Artery LigationThe piles surgeon uses an ultrasound probe to locate the arteries. A stitch is then used to tie off the artery. By interrupting the blood supply, the haemorrhoid shrivels up.
For 3rd and 4th degree piles, treatment includes:
Haemorrhoidectomy - Piles surgery is the best method for the permanent removal of more serious piles. It is usually used for 3rd or 4th degree piles or 2nd degree piles that have failed other treatments such as ligation. There are numerous ways to perform piles surgery:
- Conventional HaemorrhoidectomyHere, the piles surgeon cuts the piles from the outside and into the anal canal.
- Stapled HaemorrhoidectomyHere, the piles surgeon pushes the piles back into the anus and then cuts it off on the inside. The cut edges are closed together by titanium staples. There is lesser pain compared to conventional haemorrhoidectomy.
- Other TechniquesLaser haemorrhoidectomy or laser piles surgery uses a laser to cut the piles away in a manner similar to conventional haemorrhoidectomy. They do not offer any advantage over standard operative techniques and contrary to popular belief, are not less painful.
- Haemorrhoid Energy Transfer (HET)This is a new technique that uses a special device to burn off the piles.
Other piles treatments include cryotherapy, BICAP coagulation and direct current to shrink the piles. None of these treatments have gained widespread acceptance. For more information, visit our website on Piles Surgery.
Frequently Asked Questions (FAQ) About Piles/Haemorrhoids
Do piles lead to cancer?
Can sitting on hot surfaces cause piles?
Can stress worsen piles?
How long does piles surgery take?
How much does piles surgery cost in Singapore?
Can piles recur after surgery?
What are the best methods to prevent haemorrhoids?
Meet Our Piles/Haemorrhoids Specialist in Singapore

Dr Ho Kok Sun
Consultant Colorectal & General Surgeon
MBBS (Singapore), M Med (General Surgery) (Singapore)
FRCS (General Surgery) (Edinburgh), FAM (Singapore)
Dr Ho Kok Sun has been committed to treating piles and haemorrhoids for over a decade, through the use of both surgical and non-surgical means. Dr Ho was the past President of the ASEAN Society of Colorectal Surgeons and the Society of Colorectal Surgeons (Singapore), as well as a founding member of the Eurasian Colorectal Technologies Association. Dr Ho was actively involved in the training of medical students and residents, and has published widely in reputable journals and book chapters. He believes that treatment should always be personalised to the patient’s needs.

