Your Colorectal Health, Our Priority
With our comprehensive suite of screening services and treatment options, our experienced colorectal specialist and medical team promise you peace of mind whilst ensuring a strong and healthy colon.

Dr Ho Kok Sun
Consultant Colorectal & General Surgeon
MBBS (Singapore), M Med (General Surgery) (Singapore)
FRCS (General Surgery) (Edinburgh), FAM (Singapore)
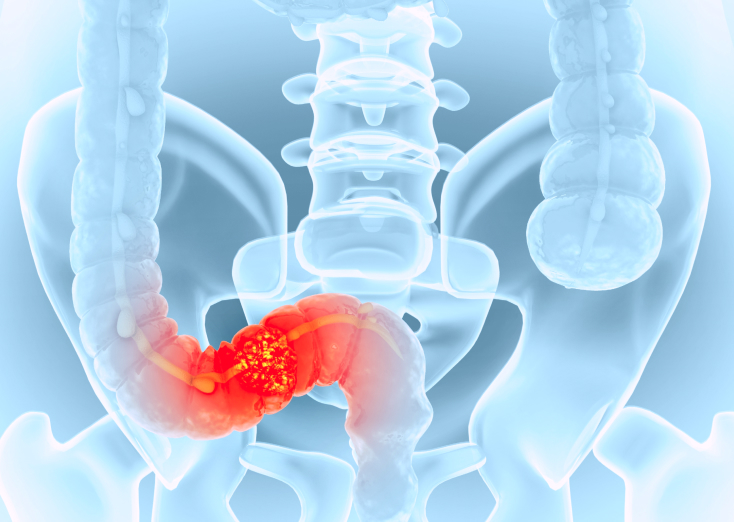
How Does Colorectal Cancer Form?
Colorectal cancer originates from the inner lining or mucosa of the colon and rectum. The lining of the Colorectal cancer develops from the inner lining of the colon or rectum. The lining of the bowel naturally renews itself over time, and occasionally, abnormal cells can form during this process.
In most cases, colorectal cancer begins as a benign (non-cancerous) growth called a polyp. Polyps are small, fleshy growths that arise from the colon lining. Many polyps are harmless, but some can slowly change over time.
Certain types of polyps, known as adenomas, have the potential to become cancerous if left untreated. As these abnormal cells continue to grow, they may develop into cancer and gradually invade deeper layers of the colon wall.
If the cancer progresses further, it can spread beyond the colon to nearby lymph nodes or other organs through the bloodstream or lymphatic system.
This gradual progression is why regular screening and early removal of polyps are highly effective in preventing colorectal cancer.
Colorectal cancer is the most common cancer in Singapore, yet one of the most preventable and treatable cancers in the early stages.
We provide risk assessments, screenings, and treatments for all patients.
How Does Colorectal Cancer Progress?
What Are The Different Stages Of Colorectal Cancer?
Our clinic is dedicated to the diagnosis and treatment of colorectal cancer.
Once the stage has been determined, we will ensure the patient is well taken care of with his or her best interests in mind.
What Are The Signs And Symptoms Of Colorectal Cancer?
It is important to note that polyps may not have any symptoms at all. Symptoms also depend on the site of the cancer and how far away it is from the end of the colon. When stools enter the colon from the small intestines, it is in a semi-solid state. As it stays and travels along the colon, the water in it gets absorbed by the colon and it becomes more solid.
As such, tumours in the right side of the colon do not usually cause much symptoms as the semi-solid stools can flow past most tumours quite easily. The cancer may bleed silently as it is mixed in the stools and cannot be seen with the naked eye. Patients with tumours here usually present late symptoms of anaemia (low blood levels). Symptoms of anaemia include tiredness, feeling breathless when walking the same distance or climbing stairs, and frequent giddiness.
At the left side of the colon, the stools are more solid. Therefore, any narrowing of the colon lumen results in the following disturbances of the bowel habit:
- The stools might seem to be narrower in size.
- Patients might also feel constipated as it is more difficult for the stools to squeeze through a narrower passageway. This might also alternate with diarrhoea or loose stools as this type of stools can pass through the narrowed passageway more easily.
- Patients might also notice blood coating the stools. As a general guide, the blood seen is usually dark red in colour.
For tumours in the rectum, the patient may have the sensation of incomplete passage of stools. This is because the presence of the tumour there imitates the presence of stools.
Other less specific symptoms include feeling of bloating and mucus in the stools. Pain is usually not a feature of colon and rectum cancer until it is at an advanced stage. One complication of the tumour is intestinal obstruction. This means that the entire passageway is blocked and the stools (and even flatus) are not able to pass through. This results in abdominal pain, distension and at a later stage, vomiting. Intestinal obstruction is an emergency medical condition.
Physical examination usually does not yield much signs unless the cancer is in an advanced stage. A hard mass in the abdomen is usually a sign of a large tumour. An enlarged liver signifies spread of the cancer to the liver. In some rectal cancers, a digital rectal examination is performed, where your colorectal doctor inserts a gloved, lubricated finger into the anus to pick up earlier cancers. As such, if your colorectal doctor thinks that you warrant a rectal examination, please do not decline or refuse for fear of discomfort or embarrassment.
It’s important to note that the early stages of colorectal cancer, as well as pre-cancerous polyps, often do not have any symptoms.
Should you experience any of these symptoms, please do not delay seeking medical attention.

What Are The Risk Factors Of Colorectal Cancer?
If you are at an increased risk of colorectal cancer, seek medical attention to determine a recommended screening schedule and personalised risk management advice.
What Are the Types of Colon Cancer Screening in Singapore?
All the different tests to examine the colon require proper cleansing of the colon. There are 3 different ways to examine the colon: colonoscopy, barium enema and computer tomography (CT) colonography (also known as virtual colonoscopy).
Speak to our experienced colorectal specialist for personalised advice on which screening method will be most suitable for your needs and preferences.
When Should I See a Colon Cancer Doctor?
It is advisable to consult a colon cancer doctor for a detailed assessment if you experience persistent symptoms lasting for more than two weeks:
- Rectal bleeding or blood in the stool
- Persistent change in bowel patterns
- Abdominal pain or discomfort (cramps or gas)
- Fatigue or tiredness
- Unexplained weight loss
What Are the Treatments For Colorectal Cancer?
The principle behind surgery for colon and rectum cancer is to remove the segment of colon or rectum with the cancer together with the adjacent area containing the lymph nodes where the cancer would initially spread. After the segment of the colon or rectum with the cancer is removed, the intestines are joined back to restore continuity so that the patient can continue to pass motion in the normal manner.
Colorectal Cancer Surgery
Surgery is the only treatment that a colorectal surgeon can offer for the definite cure of colon and rectum cancer. Other treatment modalities such as chemotherapy and radiation therapy may be used as additional treatment in reducing the risk of recurrence but do not consistently offer a cure.
In cases where the tumour is very close to or invading the anus, the rectum may have to be removed to ensure that the cancer is completely excised.
In certain cases of rectal cancer, the colorectal surgeon may also decide to utilise a temporary stoma. This is because the joint (anastomosis) for the colon to anus has a higher rate of non-healing. Having the temporary stoma acts to divert stools away from the anastomosis so that even if it does not heal properly, there will not be any leakage of stools into the abdominal cavity and cause major complication and infection. In these cases of temporary stoma, the stoma will be closed about 6 weeks to 3 months later.
Non-Surgical Treatments For Colorectal Cancer
Chemotherapy
Chemotherapy is used as an adjuvant therapy. This means that it is used in support of surgery which is the main modality of treatment. Chemotherapy is usually recommended for stage 3 and stage 4 cancers.
Radiation Therapy
Radiation therapy is also an adjuvant therapy. It is usually used for rectal cancers that are more locally advanced. It is usually not required for colon cancer. Under certain special circumstances, your doctor may recommend chemotherapy and/or radiation therapy before surgery.
Targeted Therapy
Targeted therapy uses medications designed to act on specific molecular pathways that cancer cells rely on for growth and survival. Unlike traditional chemotherapy, which affects both cancerous and rapidly dividing normal cells, targeted therapies focus on particular proteins or genetic mutations found in tumour cells. In colorectal cancer, targeted therapy is most commonly used in advanced (stage 4) disease, and often in combination with chemotherapy.
Immunotherapy
Immunotherapy works by helping the body’s immune system recognise and attack cancer cells. It is different from chemotherapy and targeted therapy because it does not directly kill these malignant cells. Instead, it enhances the immune response against them. Immunotherapy is most commonly used in cases of advanced or metastatic colorectal cancer.
In the hands of an experienced colorectal cancer surgeon, the diseased portions of the colon or rectum can be safely removed while minimising post-operative discomfort and inconvenience.
Different Approaches to Colon Surgery
On the other hand, non-surgical treatments are usually used together to enhance the cure rates of surgery, or for controlling the cancer in cases where it cannot be cured.
A colorectal cancer surgeon will determine the most suitable treatment plan for each individual.
Post-surgery Aftercare and Recovery
After the majority of these treatment methods, patients undergo a recovery period in the hospital. During this post-surgery timespan, patients are monitored while their bowel functions gradually return to normal.
Once the patient is discharged, their specialist will likely schedule follow-up appointments for them to review their recovery progress, manage any side effects and undergo regular tests such as blood work or imaging scans.
Maintaining a balanced diet, staying physically active within limits and following medical advice can support recovery and long-term well-being. Emotional and social support from healthcare providers, family members or support groups can also play an important role in adjusting to life after treatment.
Frequently Asked Questions (FAQs) About Colorectal Cancer
Is Colon Cancer Common in Singapore?
Can Colorectal Cancer Be Prevented?
When Should You Go For a Colorectal Cancer Screening?
Is colon cancer hereditary?
What does colon cancer pain feel like?
Is colon cancer fast or slow growing?
Meet Our Colorectal Cancer Specialist in Singapore

Dr Ho Kok Sun
Consultant Colorectal & General Surgeon
MBBS (Singapore), M Med (General Surgery) (Singapore)
FRCS (General Surgery) (Edinburgh), FAM (Singapore)
Dr Ho Kok Sun has been committed to treating colorectal cancer in Singapore for over a decade. He was the past President of the ASEAN Society of Colorectal Surgeons and the Society of Colorectal Surgeons (Singapore), as well as a founding member of the Eurasian Colorectal Technologies Association. Dr Ho was actively involved in the training of medical students and residents, and has published widely in reputable journals and book chapters. He believes that treatment should always be personalised to the patient’s needs.

