Your Colorectal Health, Our Priority
With our comprehensive suite of screening services and treatment options, our experienced colorectal specialist and medical team promise you peace of mind whilst ensuring a strong and healthy colon.
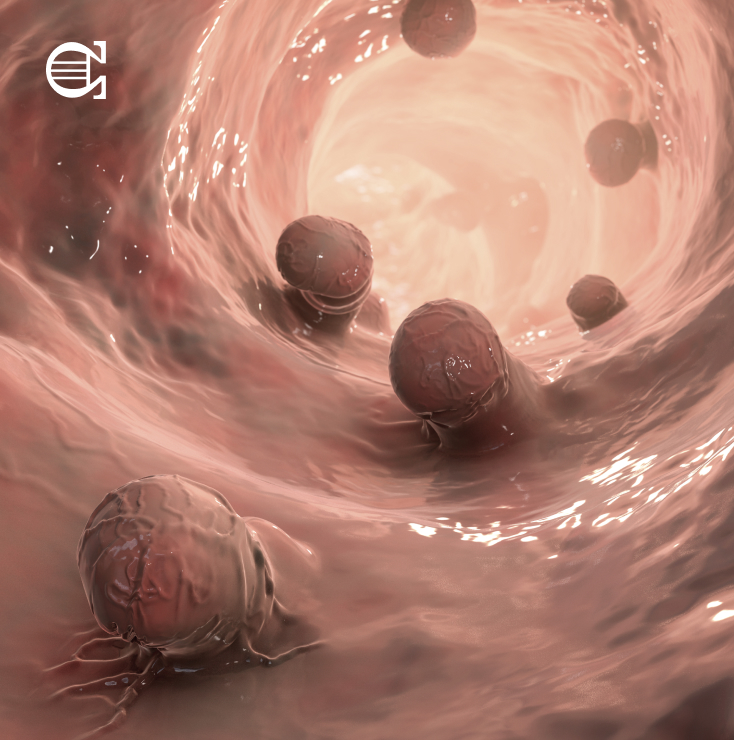
What ArePolyps?
Polyps are abnormal growths arising from the internal lining of the large intestine (colon and rectum). Some polyps are flat; others have a stalk. Polyps are one of the most common conditions affecting the colon and rectum, occurring in 15-20% of the adult population. Although most polyps are benign, certain polyps may eventually turn cancerous.
What Are The Symptoms Of The Polyps?
Most polyps have no symptoms at all and are found incidentally during an examination of the colon. This may be by colonoscopy, barium enema or CT colonoscopy. Some polyps in the rectum can be found during a rectal examination when the doctor inserts a finger through the anus and feels the polyp. Some polyps can cause bleeding, mucous discharge, change in bowel habits, or rarely, abdominal pain.
How Are The Polyps Diagnosed?
Polyps are diagnosed either by colonoscopy, barium enema or CT colonoscopy.
In the prevention of colorectal cancer, early detection and removal of precancerous polyps is key.
Contact us if you require a colon examination from a specialist.
Depending on the type and size of polyp found, your doctor will advise you on how best to manage your specific condition and risk level.
Can Polyps Recur?
A polyp does not recur after it is completely removed. However, new polyps will develop in up to 30 percent of people who previously have polyps. Patients with polyps need repeat colonoscopy to find and treat any new polyps. In some cases of large flat polyps, the endoscopist may take a more conservative approach and leave behind a bit of polyp tissue rather than removing it overzealously and end up cutting or burning a hole in the colon. In these circumstances, it is safer to leave a bit of the polyp tissues at the edges and complete the removal at a later date.
What Happens After I Have A Polyp Removed?
Your doctor would advise you of the type of polyp that was removed. Based on the nature of the polyp removed, your doctor will advise you on the subsequent follow-up. Most follow-ups would be by colonoscopy at a subsequent date and stool occult blood in between the colonoscopy.
Our Colorectal SurgeonColorectal Specialist

Dr Ho Kok Sun
Consultant Colorectal & General Surgeon
MBBS (Singapore), M Med (General Surgery) (Singapore)
FRCS (General Surgery) (Edinburgh), FAM (Singapore)
Dr Ho Kok Sun has been committed to treating colorectal cancer in Singapore for over a decade. He was the past President of the ASEAN Society of Colorectal Surgeons and the Society of Colorectal Surgeons (Singapore), as well as a founding member of the Eurasian Colorectal Technologies Association. Dr Ho was actively involved in the training of medical students and residents, and has published widely in reputable journals and book chapters. He believes that treatment should always be personalised to the patient’s needs.

